
Joint swelling, pain, erythema, warmth, and joint immobilityĪrthrocentesis with Gram stain and cultureĮlevated white blood cell count, erythrocyte sedimentation rate, and C-reactive protein Risk factors for pseudogout: hyperparathyroidism, hemochromatosis, hypomagnesemia, hypophosphatemia, osteoarthritis Risk factors for gout: male or postmenopausal female, high intake of purine-rich foods, critical illness, specific medications Tibial apophysitis (Osgood-Schlatter disease) 4, 8, 18, 26Īdolescents associated with growth spurtĬrystal-induced arthropathy (gout or pseudogout) 3, 5, 6, 9, 11, 15, 27Īrthrocentesis demonstrating crystals on microscopy Pain specific to the quadriceps or patellar tendon Quadriceps or patellar tendinopathy (jumper's knee) 3 – 5, 8, 18, 26 Tender nodule overlying anteromedial proximal tibia Patellofemoral pain syndrome (chondromalacia patellae) 3, 18, 23 – 25 Meniscal derangement or tear 5, 6, 9 – 12, 14 – 17, 19 Repetitive running, jumping, or squattingĭecreased flexibility of quadriceps and hamstrings on affected side Patellar subluxation or dislocation 3 – 5, 8ĭistal patellar apophysitis (Sinding-Larsen-Johannson syndrome) 8, 18 May report mechanical symptoms (e.g., catching, clicking)Ĭutting or twisting injury while bearing weight Tender mobile tissue band along medial joint line Injury from valgus (MCL) or varus (LCL) forceĬruciate ligament sprain or rupture (ACL, PCL) 3 – 6, 8 – 13 Physical examination tests and/or findingsĬollateral ligament sprain or rupture (MCL, LCL) 3 – 7 When the initial history and physical examination suggest but do not confirm a specific diagnosis, laboratory tests can be used as a confirmatory or diagnostic tool. Magnetic resonance imaging is rarely used for patients with emergent cases and should generally be an option only when surgery is considered or when a patient experiences persistent pain despite adequate conservative treatment. 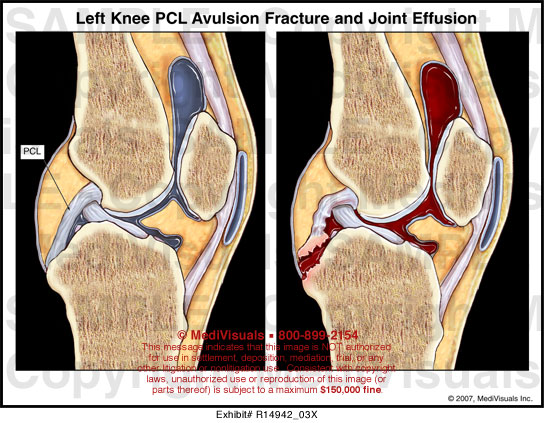
Musculoskeletal ultrasonography allows for detailed evaluation of effusions, cysts (e.g., Baker cyst), and superficial structures. Radiographic imaging should be reserved for chronic knee pain (more than six weeks) or acute traumatic pain in patients who meet specific evidence-based criteria. 
A systematic approach to examination of the knee includes inspection, palpation, evaluation of range of motion and strength, neurovascular testing, and special (provocative) tests. Patients requiring urgent referral generally have severe pain, swelling, and instability or inability to bear weight in association with acute trauma or have signs of joint infection such as fever, swelling, erythema, and limited range of motion. Key aspects of the patient history include age location, onset, duration, and quality of pain associated mechanical or systemic symptoms history of swelling description of precipitating trauma and pertinent medical or surgical history. Initial evaluation should emphasize excluding urgent causes while considering the need for referral. Knee pain affects approximately 25% of adults, and its prevalence has increased almost 65% over the past 20 years, accounting for nearly 4 million primary care visits annually.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
